It seems that so many people we know (maybe even you) have various pains and problems with their guts. We have food insensitivities or food allergies. We have irritable bowel syndrome (IBS) or Crohn’s or dyspepsia….there are lots of different maladies. As a quick indicator of the size of the problem, the US Antacid market was valued at more than $5 billion in 2022 and it’s expected to double in less than 10 years! More than 50% of Americans use some type of antacid regularly. And that’s just over the counter stuff!

Plop! Plop! Fizz! Fizz! Oh, What a Relief it Is! (Check out this commercial from 1976)
Image from: https://fphoto.photoshelter.com/image/I0000dFgOrlyy4Lw
Most of the info on the internet suggests that diet and lifestyle are the major factors in gastrointestinal maladies. Of course, that diet and lifestyle are steeped in a stew of chemicals- the unappreciated and silent marinade that damages our health.
Today I’m going to focus a little bit on IBS and the chemical exposures that play a key role.
IBS is a common ailment all over the world. Some studies estimate that more than 15% of the world’s population suffers from some level of IBS, from moderate to severe and debilitating. In the US, the prevalence is 10-25%, a huge range because it’s tough to diagnose.
What is IBS? IBS is defined as recurrent abdominal pain at least 1 day/week for over 3 months, presenting as a change in stool frequency (could be constipation or diarrhea), pain, inflammation, and bloating. IBS often co-occurs with other kinds of health issues that involve inflammation, like chronic pain or chronic fatigue; and it’s often associated with anxiety and even depression. [In a way, that’s no surprise- to be in chronic GI pain would make anyone anxious or depressed, but it’s not clear which came first….]
With such a common affliction, ever increasing over the past 20 years or so, the research into IBS has also mushroomed: 558 articles from 1980-1989; almost 2000 articles from 1990-1999 and over 7000 from 2000-2010, and over 6500 in just the last 5 years.
First, let’s take a brief tour of our GI system…
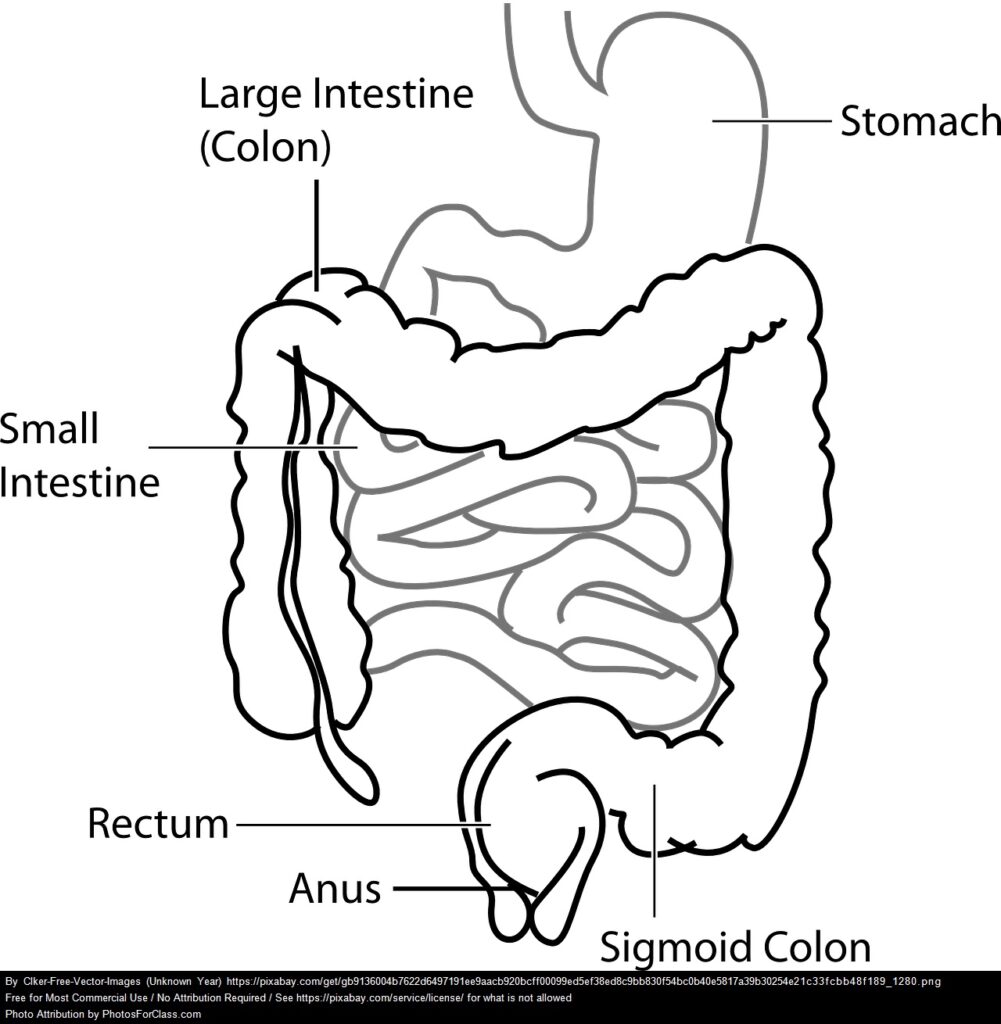
Our gastrointestinal (GI) system is fascinating- really! Our stomach and small intestine work to break down our food into the building blocks of small carbohydrates, amino acids, fatty acids, and other nutrients and absorb them into our blood stream to be used by our cells for energy and tissue repair and regeneration. Everything we need to grow and function comes from what we ingest (besides the oxygen we breathe, of course). Our colon (aka large intestine) also absorbs some vitamins and lots of water. And, this incredible system has help from a vast army (maybe 100 trillion strong!) of microorganisms- bacteria, fungi and more- called our gut microbiome— that is found in both our small intestine and colon (the stomach is a highly acidic environment and so a lot of microbes simply cannot survive there). We really are a walking, talking ecosystem.
Our microbiome does some key work for us in our colon. The microbes ferment the dietary fiber we eat to provide us with some important nutrients and protective compounds that help prevent colon cancer, fight high cholesterol and regulate our appetite [https://www.bmj.com/content/361/bmj.k2179]. Our gut microbiome also communicates with our nervous system in a two-way communication that regulates our gut function (ie. it’s motility and digestion functions) and even affects our moods and ability to handle stress. We need our microbiome and it needs us.
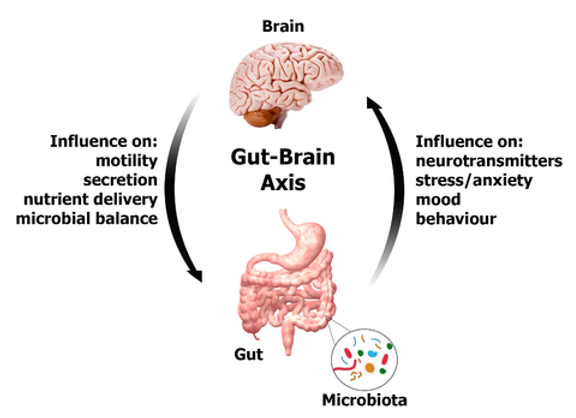
Our microbiome can become damaged or dysfunctional if it is exposed to drugs, alcohol, food preservatives, antibiotics, prescription drugs, pesticides and many other environmental chemicals. These chemicals can kill the organisms, or disrupt their metabolism so that our GI system doesn’t work right, and, if exposed to certain doses repeatedly over time, can lead to chronic conditions.
So, back to the thousands of research articles on IBS. It makes sense that there are lots of different situations that might account for IBS and other GI disorders, from alcohol use to chronic stress (and the flood of stress hormones) to a low fiber, high fat diet to…..pesticides.
A 2023 study by Dr. Shaikh and colleagues published in the Journal of Clinical Medicine (Shaikh SD, Sun N, Canakis A, Park WY, Weber HC. Irritable Bowel Syndrome and the Gut Microbiome: A Comprehensive Review. J Clin Med. 2023 Mar 28;12(7):2558. doi: 10.3390/jcm12072558. PMID: 37048642; PMCID: PMC10095554.), did a large, epidemiological analysis of almost 1.5 million people in two regions of Andalucia in Spain.

In one region, the people living there were exposed to high levels of pesticides of various sorts (it was an agricultural zone) and in the other region, people lived where there are low levels of pesticides. The scientists found that there was a significantly higher incidence and risk of IBS in people in the high pesticide region of Andalucia. This even despite differences in diet, age, socioeconomic status, smoking, other disease and disability. It was the pesticide levels, in food and the environment, that correlated with the risk and incidence of IBS.
In an even more alarming study, published in 2022 by Dr. Jessica Gama and colleagues at the Federal University of Para in Brazil, the authors concluded, after surveying the most recent scientific studies looking a chronic ingestion of low levels of pesticides, that persistent damage and chronic health conditions can arise in young children and adults. Here is a summary picture from that study that highlights the consequences:
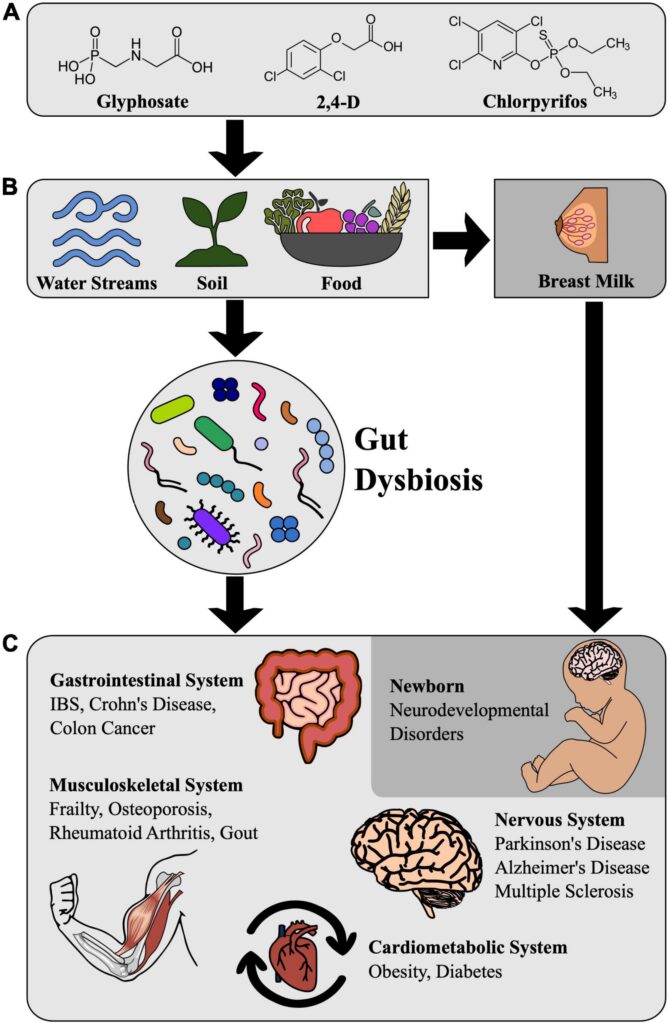
There is a lot of evidence from animal studies that low levels of pesticides of various sorts can damage the gut microbiome and lead to GI system dysfunction. Pesticides like glyphosate (in Round Up and associated with various cancers), chlorpyrifos, diazinon, aldicarb and neonicotinoids. Some of these pesticides can be washed off, or mostly washed off our food, but many, increasingly, are designed to be taken up by plants and spread inside the entire plant, so they can’t be washed off.
More than 70% of the foods we typically eat in the US, from conventional, non-organic agriculture, have residues of many different pesticides (strawberries had more than 10 pesticides, measured in a 2016 study!). Many of these chemicals remain inside the fruits and veggies, even if you wash and peel them. Tomatoes, leafy greens, corn, potatoes, sugar beets, rice, cucumbers, to name a few, are treated with systemic pesticides (these are the ones that get inside the plant). Sadly, even honey has lots of pesticides, since the honeybees get exposed to the pesticides when gathering pollen and they bring it back to the hive.
Image to the right from: https://www.kqed.org/science/1922287/70-percent-of-fruit-and-vegetables-in-the-us-has-pesticide-residue

Like every other aspect of the agrichemical industry, there is a TON of misinformation and false information that seeks to lull consumers into a false sense of safety. There ARE pesticide residues in just about everything you eat (including wine and beer) and, all the residues just add together inside your GI system. They can directly harm your microbiome, and can also injure your liver and kidney (that detoxify your blood of many pesticides) and, over time (three meals a day, your life) can add up to IBS or other conditions as an adult. Small children are much more vulnerable to acute toxicity (cuz they are smaller and also haven’t fully developed all their detox systems).
We can’t just stop eating, but here’s what you can do to try to minimize the impact of pesticides:
- Wash your produce thoroughly,
- Buy organic when you can,
- Support legal and political initiatives to reduce the use of pesticides,
- Stay informed. I recommend the Pesticide Action Network or Beyond Pesticides
I don’t know about you, but I feel like stress eating after all that!




June 20, 2023
Hi Kate!
Just what I needed to know! I think the 2 prescriptions of antibiotics have had a roll to play or caused this current condition. A 10 day and 3day dosage in about a 2 month period seems a lot–different antiobotics. Thanks! Love, MOM